Features and Benefits of Accreditation
Accreditation improves the clinical processes for the early assessment, diagnosis, treatment, and follow-up care for heart failure patients. ACC Heart Failure accredited hospitals have attained proficiency in caring for their heart failure patients and providing valuable resources within the community to help manage the disease. By adopting the ACC Heart Failure accreditation standards and committing to the implementation of process improvement methodologies, your facility will have the ability to:
- Reduce variations of care
- Enhance throughput and lower length of stay
- Sustain process improvement initiatives
- Decrease readmissions and maximize reimbursements
- Increase patient satisfaction
A Participant's Perspective
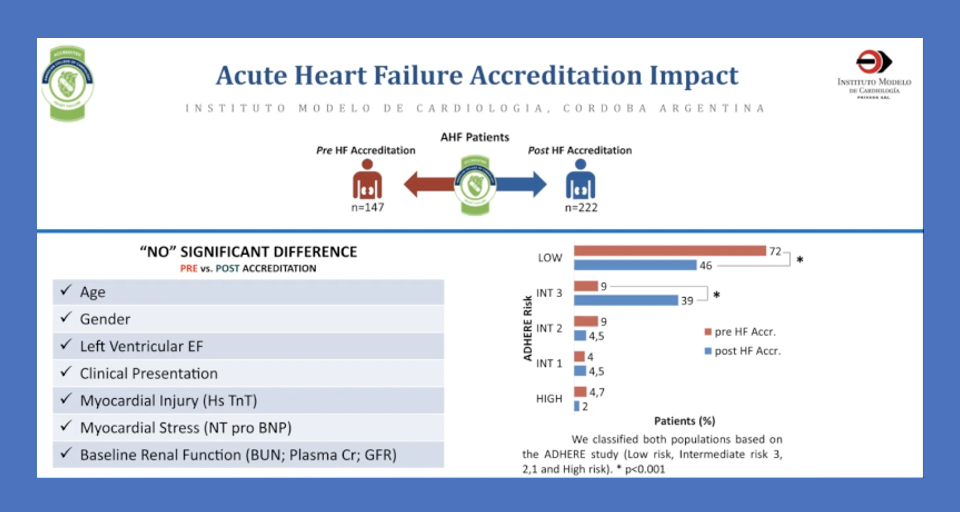
Presentation Title: Global Quality Solutions
Presenter: Dr. Javier A Sala Mercado, Instituto Modelo de Cardiologia, Cardoba, Argentina
What's Covered: In this brief video, Dr. Mercado discusses how achieving ACC Heart Failure Accreditation resulted in better patient outcomes.
Note: This video is an excerpt of a 2021 ACC Quality Summit presentation
ACC's approach to Heart Failure (HF) Accreditation is radically different from other organizations within the healthcare industry that establish specification requirements and measure compliance.
ACC takes a collaborative approach by providing feedback, education and resources to assist the facility in addressing gaps and improving processes.Partnering with your care team, the ACC experienced staff of accreditation review specialists have guided hundreds of hospitals towards achieving accreditation.
- Using measures aligned with the latest guidelines — HF Accreditation provides actionable data to support more informed clinical decisions. Through the Accreditation tool you can focus on:
- Calculated Measures for the care of your HF population
- Key performance metrics to track quality of care and identify opportunities for improvement
- Operational measures associated with patient outcomes and organizational performance
- Greater collaboration and partnership between the entire multidisciplinary HF care team
ACC's Heart Failure (HF) Partner in Care Recognition highlights outpatient provider(s) that have a solid partnership with an ACC HF Accredited facility.

To help reach quality improvement objectives, the Heart Failure (HF) Accreditation requirements are organized into process improvement efforts across nine Essential Components (EC) with the option of an Outpatient Services Designation:
Governance: Establish a multi-disciplinary committee with executive support to orchestrate program operations, ensure clinical oversight, and provide education to meet the needs of providers and staff.
Quality: Integrate continuous improvement of all aspects of care.
Community Outreach: Increase community awareness and influence behavior through education, website content, public service announcements, and partnerships with local businesses, employers, and healthcare providers.
Pre-Hospital Care: Integrate out-of-hospital interventions delivered by community healthcare providers and first responders.
HF Patient Care Management: Implement well-defined clinical processes that adhere to current guidelines, which are incorporated into the facility's order sets and flowcharts.
Observation Management: Apply targeted interventions to rapidly stabilize HF patients, reduce length of stay, and manage healthcare expenses efficiently.
Inpatient Management: Utilize a multidisciplinary approach to identify HF patients who qualify for advanced therapeutic devices or treatments while addressing additional comorbidities.
Transitions of Care: Prevent unnecessary readmissions through established care coordination, including early follow-up care and patient/family education.
Clinical Quality: Track the entire process from patient presentation through discharge and follow-up care.
Designation: Optional Outpatient Services designation based upon treatment strategies and capabilities throughout the continuum of care.
Tracking quality improvement metrics related to the care of HF patients provides valuable insight into outcomes and helps guide strategies and establish goals for the care of various HF cohorts.
To reduce data burden, facilities have the option of utilizing:
1) The Accreditation Conformance Database (ACD) within the HF tool
2) HF national/regional database or registry reports
3) HF specific facility generated reports
This flexibility allows facilities to adopt a strategy that meets the demands of the required data abstraction and collection to ensure continuous process improvement.
The ACD of the online HF Accreditation tool only captures the data that measures adherence to HF clinical practice guideline recommendations and performance standards. The required data elements are all linked to automated quality and performance metrics for the purposes of achieving HF Accreditation. Through this streamlined approach, facilities will have the ability to concentrate their efforts on process improvement efforts and the delivery of care needed at the bedside.
Although, minimal data is collected, the HF ACD and metrics still provide the following benefits:
- access to the patient level data you need to implement directed interventions
- designed for clinicians by clinicians, HF ACD keeps patient flow at the center of data aggregation
- provides metrics with drill-down capability
A sustainable and comprehensive strategy to process and quality improvement is your blueprint for a successful accreditation. Accreditation provides a foundation for promoting long-term and optimal value for the delivery of healthcare services to patients. By ensuring all personnel and departments speak the same language and use the most up to-date protocols and policies, you enhance efficiencies and eliminate variations in patient care. Consequently, you’re able to improve patient outcomes and financial performance. HF Accreditation helps your facility:
- Streamline patient care to ensure continuous positive clinical trajectory and throughput to reduce the length of stay
- Inclusion of updated guideline directed medical therapies, resources, and shared practices
- Identification of patients eligible for cardiac rehab and advanced therapies
- Build collaborative relationships with pre-hospital and post-discharge providers
- Enhanced transitions of care models to detect precipitants and reduce risk of readmission

