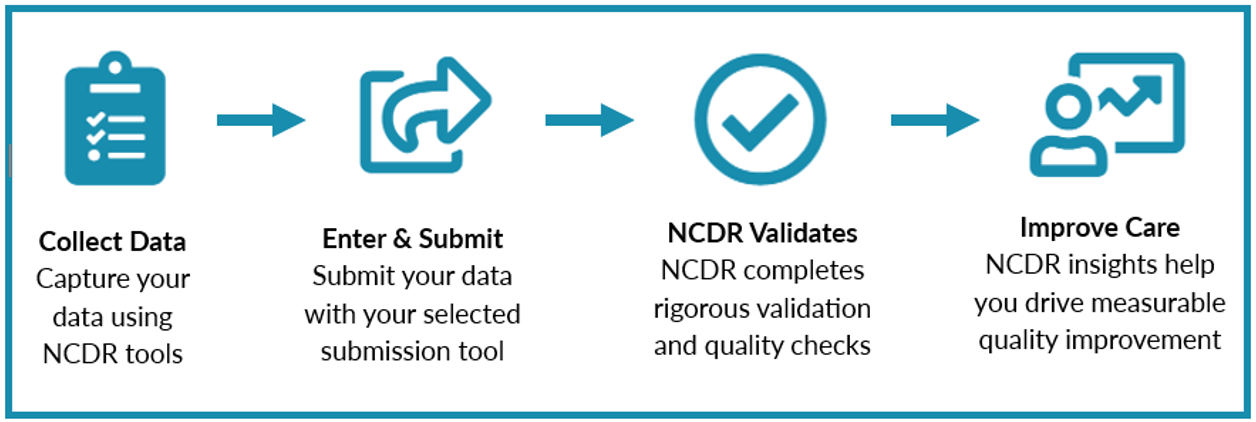
The NCDR Data Journey
The NCDR transforms your facility's clinical outcomes data into trusted, actionable intelligence that elevates cardiovascular care. Every step is engineered to deliver data you can rely on with confidence.
How to Connect with ACC
New to NCDR
If your facility is not yet enrolled, request information to connect with our team about eligibility, timeline and next steps.
General Support
Not yet a NCDR participant? Please submit your inquiry here, our team will be happy to assist you.
Learn More
Want to see how your data becomes meaningful insights? View below to see how NCDR supports you through your journey.
NCDR offers a complimentary online data collection tool, allowing sites to enter patient records directly through the secure NCDR portal. Additional support resources include:
- Data Collection Forms
- Data Element Dictionaries
- Data Inclusion Companion Guide
If you do not use the complimentary online data collection tool, you may choose an NCDR certified software vendor as an alternative data collection solution that also supports data submission to NCDR.
Data abstraction can be completed at your facility, or you can select a Data Abstraction Provider to assist you.
NCDR's submission process functions to ensure data is complete and accurate. Submissions to the data warehouse result in a Data Quality Report (DQR), which validates your data based upon thresholds and completeness to ensure operation clarity and confidence.
Each NCDR registry captures specific insights designed to help hospitals transform data into meaningful quality improvement. Click Here to explore the registry that best fits your needs and learn what data it collects. NCDR provides performance metrics on a quarterly basis.

